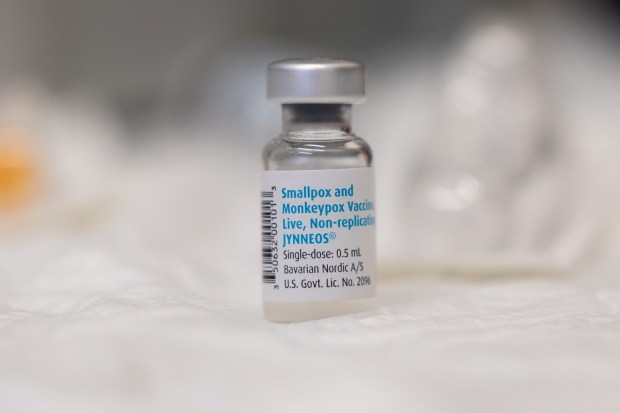
Weekly cases of mpox, the virus formerly known as monkeypox, have remained in the single digits in Chicago this year. That’s much lower than during the virus’s outbreak two years ago, which at its peak saw cases reach over 140 in a week, but “it’s concerning that it’s still circulating” in the U.S., said Dr. Aniruddha Hazra, associate professor of medicine and director of the Infectious Diseases Fellowship Program at the University of Chicago.
And now, the U.S. has seen its first case of another more virulent strain of the virus, known as clade I. This clade first began to spread in the Congo and has killed over 600 people, according to numbers in a September study. Cases have since been reported in other countries such as the Philippines, Sweden and Thailand.
The U.S.’ first case was recorded in California mid-November, with the patient reportedly experiencing mild symptoms.
Funding and resources for fighting mpox — which causes a blister-like rash and, in the worst cases, death — have declined in the U.S. But in Chicago, efforts to vaccinate vulnerable populations and educate them about mpox have remained in place.
During the first outbreak, the virus disproportionately impacted gay and bisexual men and other men who have sex with men. In this newer outbreak, researchers studying mpox transmission in a province of the Congo noted this summer that “heterosexual transmission could be driving the transmission rates.”
When it comes to handling mpox, “the onus is on local and state jurisdictions to develop and implement their own mpox responses,” Dr. Tim Menza, medical director, public health at the Seattle and King County Sexual Health Clinic, said in an email.
The Chicago Department of Public Health, which has been given $1.66 million in total from the federal government for its mpox response, funds vaccination events, tracks cases and has held weekly meetings about the virus since 2022 with health leaders and organizations ranging from the Chicago Black Gay Men’s Caucus to Howard Brown Health.
Howard Brown, a health care nonprofit that serves the LGBTQ+ community, used to hold vaccine clinics that included the mpox vaccine, but has since stopped due to “changes in operations,” according to Terra Campbell, its associate director of community relations. The nonprofit continues to offer the vaccine via scheduled appointments, and it’s unclear “if or when we plan to return” to public vaccination clinics, she said.
Although Howard Brown offers its vaccines independently, the city’s health department works with hospitals Rush University Medical Center and the University of Illinois Chicago to administer mpox vaccines across the city. This is an “unusual” collaboration with the city department, Rush spokesperson Polly Tita wrote in an email. It began at the start of COVID-19 with the aim of responding to health emergencies ranging from COVID to a recent measles outbreak to mpox, said Dr. Elizabeth Davis, who leads Rush’s vaccine outreach efforts.
The hospitals are focused on bringing vaccines to people, particularly in communities that face barriers to access including residents of the South and West sides, where there are fewer pharmacies for people to get vaccinations, Davis said.
As a result, “we do community vaccine events all the time,” Davis said. One such vaccine was held at Latino and HIV-focused nonprofit Calor at the end of October, where Calor also provided free HIV testing.
Organizations such as Calor help medical providers reach groups who most need the vaccine, said Calor’s program manager of prevention and education devices, Alfredo Flores. Calor acts as a wraparound service to connect people to long-term care, he said.
Calor itself doesn’t get city dollars, and instead receives most of its funds from the AIDS Foundation, of which it is an affiliate.
People who are immunocompromised, including those with unmanaged or advanced HIV, are “most vulnerable” to mpox, Hazra said. Of the total tens of thousands of cases, 38% were people with known HIV, according to a Centers for Disease Control and Prevention weekly report from May 2023, although the risk extends to people who don’t know they have HIV.
The city health department’s outreach approach is “aligned with” the CDC’s mpox vaccine recommendations, which “do not spell out specific focus on people living with HIV,” department spokesperson James Scalzitti wrote in an email. When asked about its efforts to reach people with HIV, Scalzitti said that the city has reminded HIV case managers and care coordinators to speak with clients about the mpox vaccine.
Another organization that has worked with people with HIV around mpox is the HIV Hub, which is run by the AIDS Foundation Chicago in partnership with Center on Halsted to help LGBTQ+ people with or without HIV navigate health care.
When the HIV Hub gets calls from people asking about mpox this year, “out of five calls, one individual would want to remain anonymous but other participants are open with sharing who they are,” said Melanie Cross, senior manager of care systems management at Chicago’s AIDS Foundation and oversees the HIV Hub, which gets most of its funding from the CDPH, she said. “In the last year, stigma has been reduced.”
There have been some changes to city and nationwide efforts to fight mpox. For example, Chicago’s health department and other city health departments around the country have stopped updating vaccination data “due to the contraction of resources to do mpox work,” according to Menza, medical director of public health at the Seattle and King County Sexual Health Clinic. The CDC stopped reporting vaccine coverage data by state in January.
“CDPH’s efforts have not remained the same,” Scalzitti said. The city’s first mpox response was a “collaboration between multiple CDPH bureaus,” but as cases became less frequent, the effort was led by the city’s Syndemic Infectious Disease Bureau and Immunizations Bureau, “with assistance from other bureaus as needed,” he said.
When cases of clade 1 began to break out globally, this assistance was “ramped up,” Scalzitti said. “Efforts are consistently adjusted,” he said, citing education and outreach.
Communication across health departments nationwide has also died down, making it “quite hard to know what other cities are doing and how successful they are,” Menza said.
According to Davis, the partnership between UIC, Rush and the CDPH has has not seen much decrease in resources or staffing.
Compared with other conservative states and cities, Chicago has done a “great job because the health department has led (mpox) efforts,” Flores said. There are problems when “health departments don’t get involved in the administration process and hospitals and clinics are left on their own,” he said.
“There are cities (and states) that do not want to talk about sexual health or mpox, because mpox is related to sexual health” and LGBTQ+ issues, he said, citing Texas and Florida as examples. “Stigma plays a big role in people wanting access to care.”
Another potential issue when it comes to vaccine access is that the vaccine Jynneos has since been commercialized and will no longer be free. This could make the vaccine unaffordable for those who are uninsured, say activists. “Federal agencies are working to incorporate Jynneos vaccine into their programs to support broad access to this vaccine, including among people who are uninsured and underinsured,” according to a notice on the CDC website.
There are also outstanding questions about the spread, including how long the vaccine immunizes people for, said Dr. Kenneth Mayer, professor of medicine at Harvard Medical School and director of HIV Prevention Research and Beth Israel Lahey Health.
“Let’s do some preemptive investments,” Jeremiah Johnson, executive director of advocacy organization PrEP4All, said in a June interview. “Let’s make sure that a free vaccine is available, particularly in communities that are going to be uninsured.”
Jade-Ruyu Yan is a freelance writer.